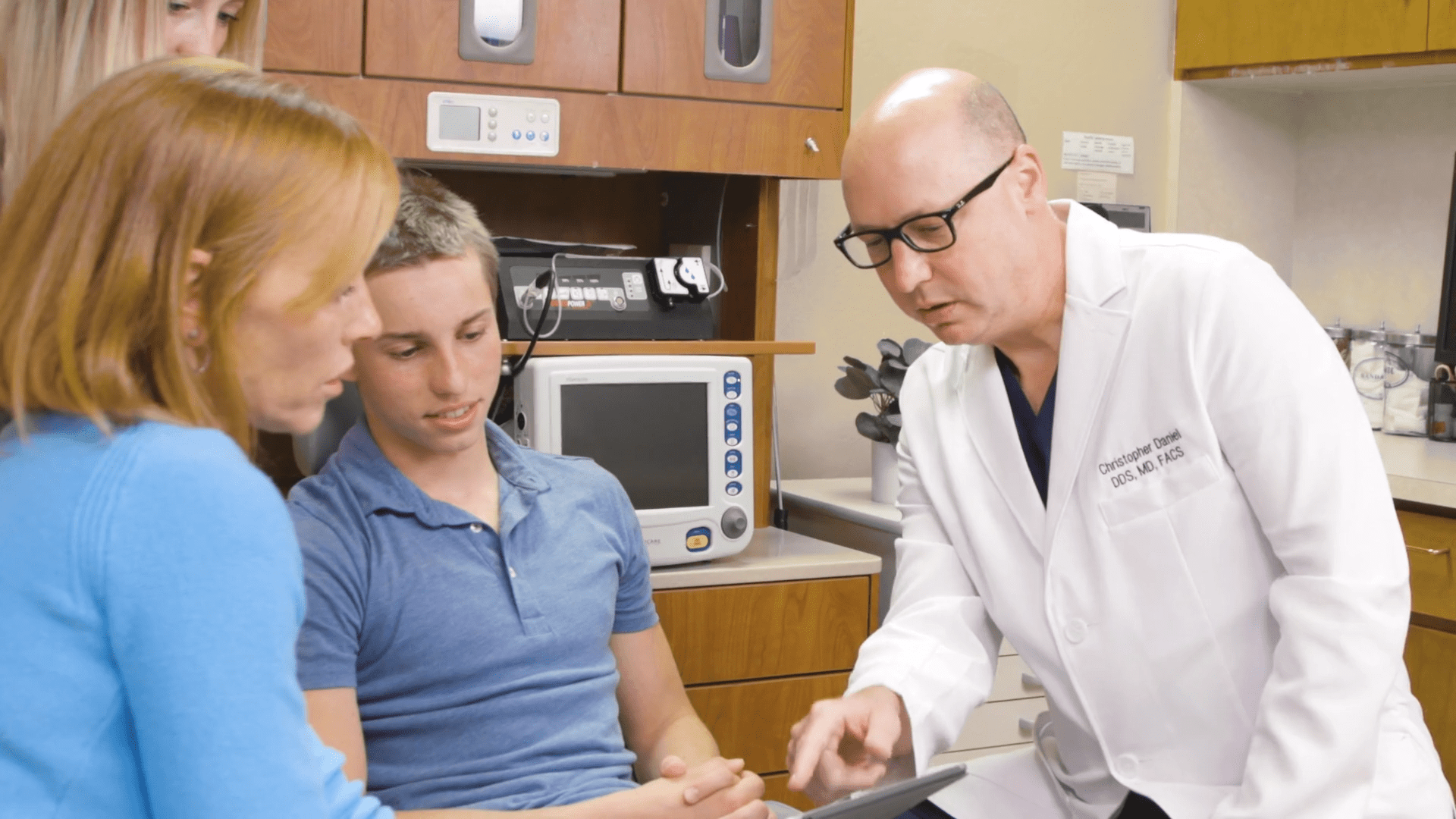
Obtaining powerful stem cells from wisdom teeth for the potential treatment of future illness and disease is now a reality.
Wisdom teeth contain powerful stem cells
We are on the cusp of achieving truly personalized medicine, and stem cells are at the heart of it. Research has suggested that the most potent stem cells for use in medical treatments come from young people between the ages of 13 and 24. This means that collecting and storing stem cells from your child’s wisdom teeth today has the potential to protect their health tomorrow. Stem cells found naturally in wisdom teeth have the proven ability to regenerate and repair diseased tissue and organs.
GMP-compliant laboratory & storage facility
Our Stemodontics laboratory and storage facility meets and exceeds Good Manufacturing Practice (GMP) standards. We follow strict regulatory requirements to ensure the health, safety, and well-being of our team, partners, and members.
Stemodontics in the news
Explore the articles and posts of Stemodontics and stem cells in the news to learn more about the possibility of stem cells and regenerative medicine.
Current stem cell research
Discover what stem cell researchers are working on today in their mission to discover new treatments and therapies for patients.
Find a provider
Locate a trusted Stemodontics provider near you.